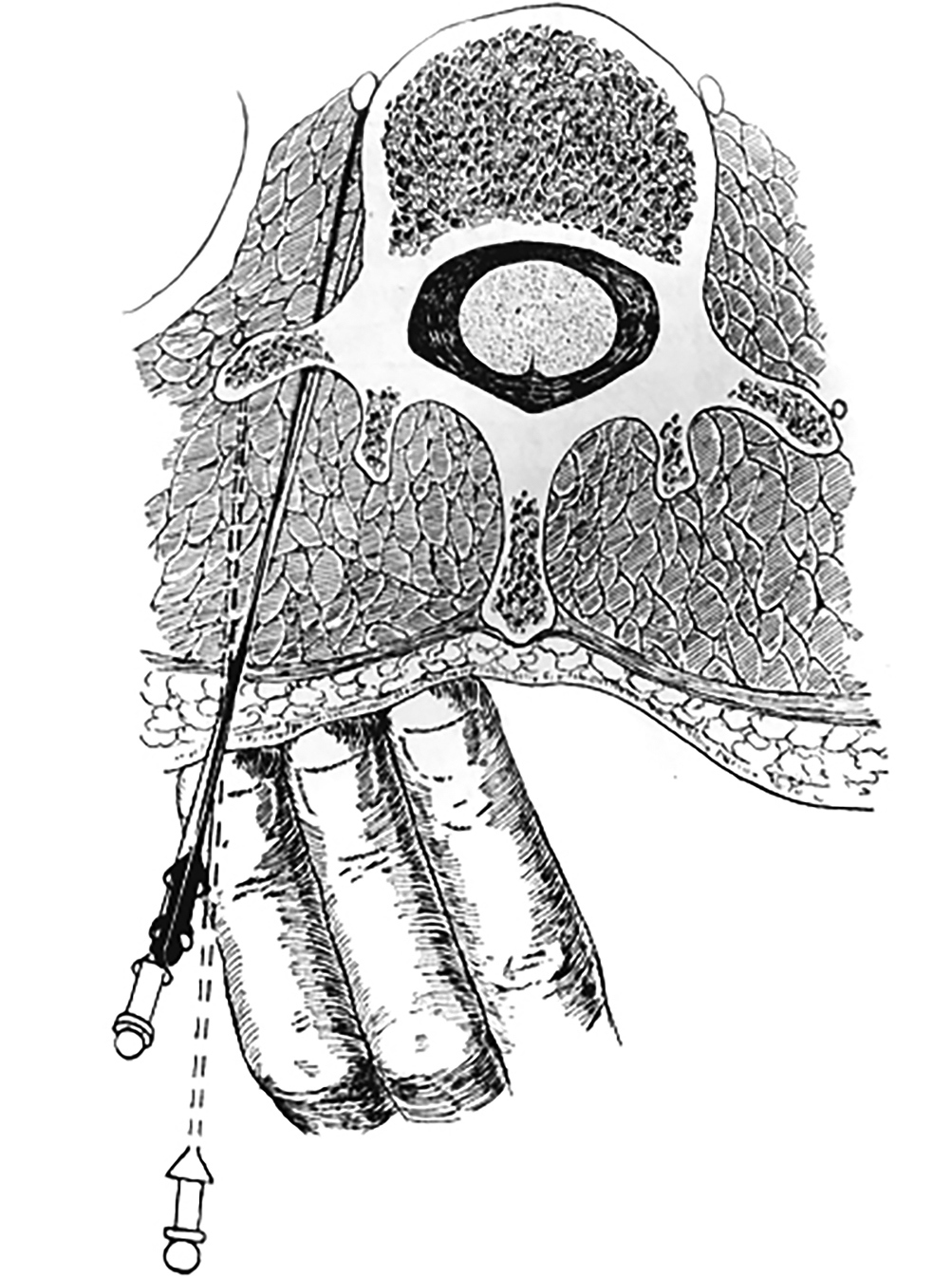
In 1924, Australian surgeon Norman D. Royale, MD delivered the keynote john B. Murphy Oration in Surgery at the ACS Clinical Congress on an unfamiliar topic—sympathectomy.
Along with his colleague John I. Hunter, MD, Dr. Royale proposed severing the sympathetic nerve bundle as it exited the vertebral column to treat spastic paralysis.1 The presentation inspired William J. Mayo, MD, FACS, and ACS founder Franklin H. Martin, MD, FACS, to visit Australia, learn the intricacies of the new technique, and bring it back to the US, where The New York Times announced hope for a cure of this intractable condition. In disproving its efficacy against paralysis, physicians discovered its utility in redressing peripheral arterial disease (PAD), where it flourished as a mainstay of treatment for the next 20 years.
Physicians had conceived a very rough equivalent of the autonomic nervous system since at least the Middle Ages, with anatomical investigations in the 16th century further defining their course. Anatomist Jacques B. Winslow—credited with first documenting the existence of the foramen that bears this name—called them “sympathetic” in 1752.
In 1851, French physiologist Claude Bernard reported that severing a sympathetic nerve resulted in the dilation of blood vessels. His countryman, surgeon Mathieu Jaboulay, performed the first known sympathectomy when he extirpated pelvic rami to relieve pain in a patient’s lower urinary system. Dr. Jaboulay’s student, vascular surgeon and physiologist René Leriche, conducted the first sympathectomy for peripheral vascular disease in 1913.2 Dr. Leriche’s work, however, remained confined to France; while later seen as inspiring and revelatory, it initially had only local effect.
Peripheral vascular disease at the time had few therapeutic options. Scottish surgeon John Hunter had demonstrated the value of ligation, but that therapy was appropriate only for aneurysms and carried a significant risk of amputation. What we now call atherosclerotic vascular disease was becoming increasingly common in 20th century America as deaths from infectious etiologies, such as cholera and tuberculosis, fell and lifestyle changes led to calcified vessels throughout the body. Surgeons and other physicians quickly learned to diagnose the condition but lacked drugs or interventions to remedy it.
Drs. Martin and Mayo brought sympathectomy back to Chicago, Illinois, and Rochester, Minnesota, respectively, where surgeons quickly demonstrated its futility in curing paralysis. But Mayo Clinic physician George E. Brown, MD, had observed experiments by neurosurgeon Alfred W. Adson, MD, and noted that while paralysis remain unchanged, the limb on the side where Dr. Adson operated was markedly warmer than the contralateral extremity. Dr. Brown, already interested in PAD, hypothesized that the operation might benefit those patients instead, and performed a number of controlled experiments on animals to test this theory. In March 1925, Drs. Brown and Adson performed the first sympathectomy for vascular disease in a patient suffering from Raynaud’s disease, curing him (see Figure 1, below).3