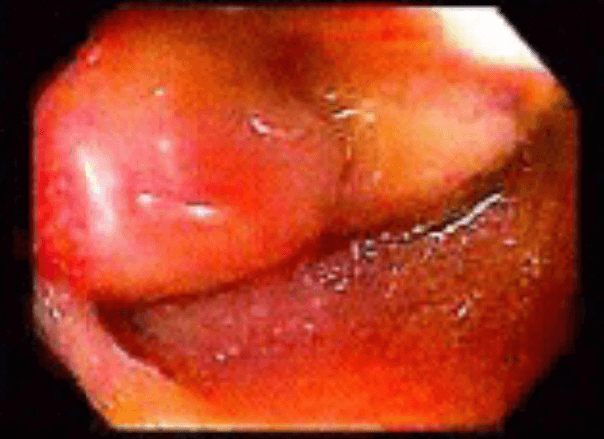
Discussion
Isolated injuries to the CBD following blunt abdominal trauma in pediatric patients are rare. Management of this injury has been described after cholecystectomy in the adult population, but literature is limited regarding the pediatric trauma patient.1,2 To our knowledge, this case is the first CBD avulsion managed nonoperatively using a rendezvous procedure in the pediatric trauma population.3
Previous reports make mention of successful use of the rendezvous procedure for pancreatic duct injuries.4 However, a fully transected duct repaired using the rendezvous procedure has never been fully described. Given the proximity of the injury to the pancreatic head, the surgical team was concerned that our patient would require a pancreaticoduodenectomy. With the assistance of our gastroenterology and interventional radiology colleagues we were able to avoid a major operation. Long-term complication rates are unknown, but our patient has done extremely well and has had no complications from this procedure. Our case illustrates that pediatric patients with a complete CBD avulsion may be successfully managed with an endoscopic and transhepatic rendezvous technique, avoiding a major operation.
Conclusion
Pediatric patients with a complete CBD avulsion may be successfully managed with an endoscopic and transhepatic rendezvous technique, avoiding a major operation.
Lessons Learned
Common bile duct avulsion in pediatric trauma can be managed nonoperatively. Early consultation of gastroenterology and interventional radiology specialist may aid in caring for this rare injury.
Authors
Paul McGaha, MD
University of Oklahoma Health Science Center
Department of Surgery
Oklahoma City, OK
William Vanlandingham, MD
University of Oklahoma Health Sciences Center
Department of Radiological Sciences
Oklahoma City, OK
John Maple, DO
University of Oklahoma Health Sciences Center
Department of Gastroenterology
Oklahoma City, OK
Jeremy Johnson, MD
University of Oklahoma Health Science Center
Department of Surgery
Oklahoma City, OK
Correspondence
Paul McGaha, MD
Department of Surgery
800 Stanton L. Young Blvd
Andrews Academic Tower, Suite 9000
Oklahoma City, OK 73104
Phone: 903-780-2062
E-mail: Paul-mcgahaii@ouhsc.edu
Meeting Presentations
5th Annual Pediatric Trauma Society Meeting
Houston, TX
November 2018
Disclosures
The authors have no conflicts of interest to disclose.
References
- Schreuder AM, Booij KAC, de Reuver PR, et al. Percutaneous-endoscopic rendezvous procedure for the management of bile duct injuries after cholecystectomy: short- and long-term outcomes. Endoscopy. 2018 Jun;50(6):577-587.
- Fiocca F, Salvatori FM, Fanelli F, et al. Complete transection of the main bile duct: minimally invasive treatment with an endoscopic-radiologic rendezvous. Gastrointest Endosc. 2011;74(6):1393-1398.
- Odemis B, Shorbagi A, Koksal AS, et al. The "Lasso" technique: snare-assisted endoscopic-radiological rendezvous technique for the management of complete transection of the main bile duct. Gastrointest Endosc. 2013;78(3):554-556.
- Ishii K, Itoi T, Tsuchiya T, Mukai S, Kohno M. EUS-guided pancreatic duct rendezvous in a child with traumatic pancreatic duct disruption. Gastrointest Endosc. 2014;80(3):519-520.